Advances in T cell receptor gene transfer for immunotherapy
Judy Wai-Ling King, Graham P. Wright and Hans J. Stauss
Department of Immunology, Royal Free Hospital, University College London, UK
Accepted 10 November 2008
Published 27 November 2008
Summary
Adoptive T cell transfer has seen clinical success in the treatment of both malignancies and viral infections. However, one of the main limitations of this strategy has been the difficulty in producing sufficient quantities of antigen-specific T cells. In addition, donor lymphocyte infusions are commonly associated with graft-versus-host disease (GvHD), which carries with it significant morbidity and mortality. Retroviral T cell receptor (TCR) gene transfer is an attractive new strategy by which large numbers of autologous, antigen-specific T cells can be generated, since the TCR is the sole determinant of T cell specificity. The introduced TCR specificity can be targeted against viral antigens or poorly immunogenic targets such as tumor associated antigens, and recent clinical trial data has demonstrated the feasibility of this technique in melanoma patients. Furthermore, TCR gene transfer also has the potential to generate antigen-specific regulatory T cells. This review will focus on recent advances in the field of TCR gene transfer and explore the potential clinical applications of this strategy.
Keywords
Immunotherapy, t cell receptor (tcr), gene transfer, cancer
Introduction
Adoptive T cell transfer has seen clinical success in the treatment of both malignancies and viral infections. However, one of the main limitations of this strategy has been the difficulty in producing sufficient quantities of antigen-specific T cells. In addition, donor lymphocyte infusions are commonly associated with graft-versus-host disease (GvHD), which carries with it significant morbidity and mortality. Retroviral T cell receptor (TCR) gene transfer is an attractive new strategy by which large numbers of autologous, antigen-specific T cells can be generated, since the TCR is the sole determinant of T cell specificity. The introduced TCR specificity can be targeted against viral antigens or poorly immunogenic targets such as tumor associated antigens, and recent clinical trial data has demonstrated the feasibility of this technique in melanoma patients. Furthermore, TCR gene transfer also has the potential to generate antigen-specific regulatory T cells. This review will focus on recent advances in the field of TCR gene transfer and explore the potential clinical applications of this strategy.
Adoptive T cell transfer for tumor immunotherapy
Adoptive transfer of allogeneic hematopoietic stem cells (HSC) is an established treatment for hematological malignancies. Donor T cells are responsible for mediating the graft-versus- leukemia effect, but this is associated with graft-versus-host disease in up to 50% of transplant recipients. One of the most exciting applications of TCR gene transfer is the ability to generate autologous T cells that recognize leukemia or tumor antigens (Figure 1). There are a number of tumor associated antigens (TAA) that are being evaluated as targets for the immunotherapy of malignancies. However, while they are over-expressed on tumors, they are also expressed on normal tissues, albeit at low levels. Autologous T cells which naturally recognize tumor antigens with high affinity are subject to tolerance mechanisms such as deletion or anergy. Hence, although autologous T cell responses against tumor antigens can be detected in patients with malignancies, they are generally of low avidity. Since it has been shown that the transduced T cell population demonstrates the same functional avidity as the original parent T cell from which the TCR genes are cloned, one of the advantages of TCR gene therapy is that a high avidity TCR can be selected for transfer into target T cells. There are several methods by which high avidity cytotoxic T lymphocytes (CTL) specific for TAAs can be generated. Immunization of HLA transgenic mice, the allo-restricted approach, in vitro mutagenesis of TCRs, and in vitro selection using phage display have been used to generate TCRs with increased peptide/MHC binding affinity.
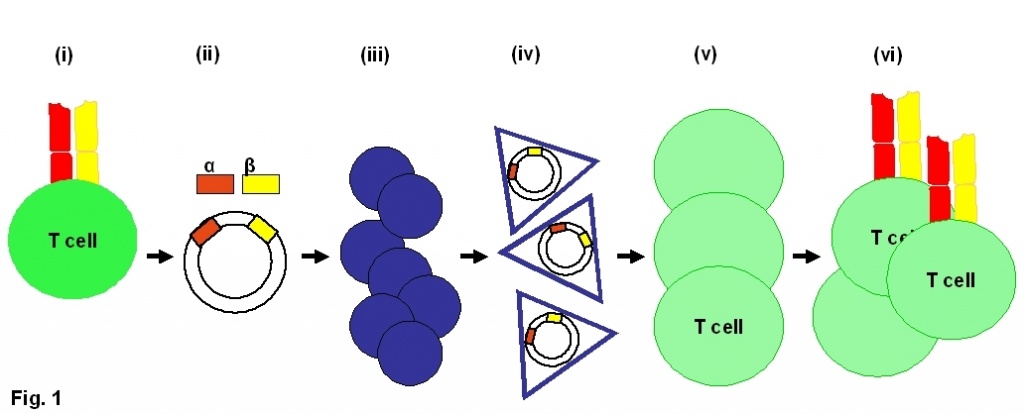
Figure 1. TCR gene transfer.
(i) A T cell bearing the appropriate TCR is identified, (ii) the alpha and beta TCR chains genes are isolated and cloned into a retroviral vector, (iii) the vector is used to transfect a packaging cell line which produces viral particles containing the genes of interest: (iv). (v) Target T cells are transduced with the recombinant viral particles; (vi) when the genes integrate into the host DNA the target cells express the desired TCR.
Transduced T cells have been shown to contribute to tumor clearance in murine models , and the first clinical trial of TCR gene transfer was recently reported. Retroviral gene transfer was used to transduce peripheral blood lymphocytes taken from patients with melanoma, with the genes encoding the α and β chains of a TCR with specificity for a MART 1 peptide presented by HLA-A*0201. The 17 patients in the gene transfer study were lymphodepleted prior to receiving autologous T cells transduced with the MART-1 TCR. The engineered T cells persisted in 15 patients, and the two patients with the highest levels of circulating anti-melanoma T cells showed objective regression of metastatic lesions and remained in remission 18 months after treatment. The results of this study prove that retroviral TCR gene transfer can be used to confer anti-tumor specificity upon a large number of autologous T cells, and that these T cells can engraft in patients and persist at high levels long term.
TCR gene transfer to generate anti viral T cells
A further application for TCR gene transfer is to generate virus-specific T cells for the treatment of immunosuppressed patients who have undergone HSC transplantation. After GvHD, post transplant viral infection is the next major cause of morbidity and mortality in transplant recipients. Adoptive T cell transfer has been shown to be an effective treatment for cytomegalovirus (CMV) and Epstein-Barr virus (EBV) infection in transplant recipients. Donor-derived CMV specific CD8 T cells which had been expanded in vitro were then infused into HSC transplant recipients with good effect. Similarly, donor-derived EBV specific T cell lines have been used to treat EBV related post-transplant proliferative disease. However, the major limitation of this strategy is that it is not possible to generate virus-specific CTL from all HSC donors using in vitro expansion techniques. TCR gene transfer has the ability to overcome this obstacle and confer upon donor T cells TCR specificities that are not present in the endogenous donor repertoire. This technique also has the advantage of generating large numbers of virus-specific CTL far more rapidly than standard in vitro expansion approaches, which would be of clear benefit in a clinical scenario where a patient presents acutely with significant morbidity. While clinical trial data is still pending, this strategy has great potential for the treatment of viral infections in HSC recipients.
Augmenting TCR gene transfer
In recent years, several groups have explored the means by which TCR gene transfer can be optimized. Modern vector designs aim to increase exogenous TCR expression on target cells by combining α and β chains in a single vector linked by viral self cleaving 2A sequences, rather than internal ribosome entry sites. Codon optimization of TCR gene sequences has also been shown to result in increased TCR expression in human CD8+ T cells, and increased antigen-specific IFNγ release.
In parallel with these vector modifications, recent research efforts have been directed towards increasing the preferential pairing of exogenous α and β chains with each other. It has been demonstrated that exogenous TCRs are able to mispair with endogenous TCR chains (Figure 2). Any mispairing may reduce the expression density and hence the efficacy of the desired TCR, since the density of TCR expression on the cell surface has been shown to correlate with avidity. A number of strategies have recently been employed to address this issue. TCRs have been engineered to include an additional cysteine residue in the constant regions of the α and β chains, resulting in the formation of a second disulphide bond between them. T cells transduced with cysteine-modified receptors showed increased tetramer binding, secreted more cytokine, and showed increased antigen specific lysis when co-cultured with specific tumor cell lines, compared with T cells expressing wild type TCR. Hybrid TCRs have also been designed to incorporate murine constant regions and human variable regions. These hybrid TCRs show reduced mispairing with fully human TCRs when introduced into human T cells, combined with superior cell surface expression and biological activity. However, there is a possibility that a human host will mount an immune response against the murine component of such a TCR. In the same way that murine monoclonal antibodies have become increasingly humanized for clinical use, it is likely that murinization of the TCR constant region will be minimized to reduce its immunogenicity, if this strategy is to be used in a clinical setting.
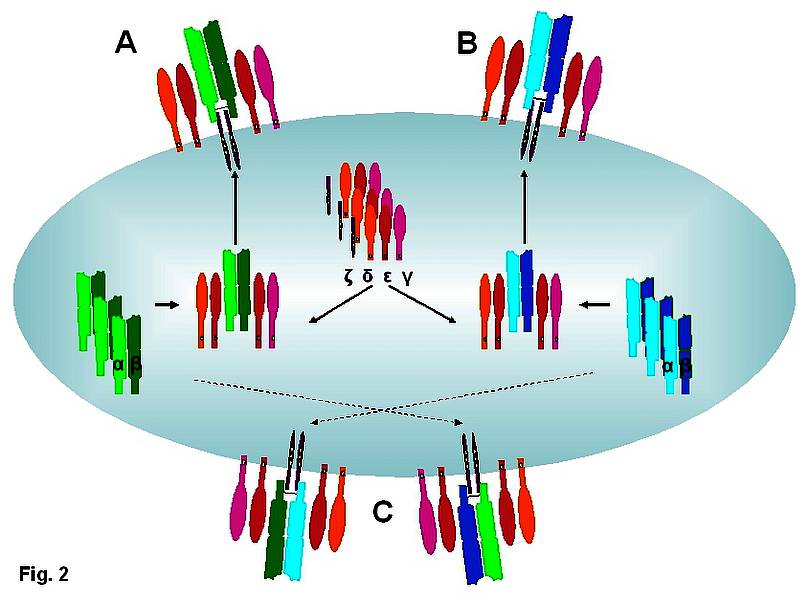
Figure 2: exogenous and endogenous TCR chains compete for CD3 molecules for surface expression, and can mispair to form mixed dimers of unknown specificity. TCR α and β chains must form a complex with the ζ,δ,ε and γ CD3 chains in order for the TCR to be expressed on the cell surface. Following retroviral TCR gene transfer, there is competition between the endogenous TCR (A) and the exogenous TCR (B) for CD3. Increasing the availability of CD3 chains could increase the density of expression, and hence functional avidity, of the exogenous TCR. C: mispairing of endogenous and exogenous TCR chains leads to mixed dimer formation. These TCR have the potential to be autoreactive, and also reduce the CD3 available for expression of the desired TCR (B).
Strategies such as murinization of constant domains and cysteine modification of TCR chains reduce mispairing and increase the "strength" of a TCR. Recent data has shown that "strong" TCRs are expressed at high levels following retroviral gene transfer, whereas "weak" TCRs are poorly expressed because they compete poorly against the endogenous TCR repertoire for CD3 molecules. Research is ongoing into whether there are specific amino acid sequences in the TCR constant domain that contribute towards "strength." An alternative strategy that is currently being investigated is the cotransduction of TCR along with the genes encoding the CD3 complex. Endogenous and exogenous TCR chains are in competition for a limited pool of CD3 molecules, and exogenous TCR chains are likely to be present in excess, since their production is under the control of a retroviral promoter. The expectation would be that cotransducing with both TCR and CD3 molecules would increase the availability of CD3 molecules, which would have a more profound effect on expression of the exogenous TCR whose α and β chains are present in excess.
Safety concerns
Although there is no evidence of off-target toxicity in murine models to date, it has been demonstrated that exogenous TCR are able to mispair with endogenous TCR chains, resulting in the expression of TCRs that have not undergone thymic education. These TCR, with unpredictable specificities, have the potential to be autoreactive. The strategies described above have been employed to both reduce mispairing and to increase expression of the desired TCR. Research is ongoing into alternative means by which the risk of mispairing may be reduced. It has recently been shown that TCR α and β chains which have each been linked to a CD3ζ chain did not mispair with endogenous TCR chains in a Jurkat T cell model. Since γδ TCR chains cannot mispair with αβ TCR chains, transferring αβ TCR chains into γδ T cells should not result in any mispairing, and has previously been shown to result in the expression of exogenous αβ TCR which produce cytokine and lyse target cells in an antigen-specific manner. Transduction of viral-specific T cells is a strategy by which the potential number of mixed dimers can be reduced; since anti viral responses consist of T cells with a restricted TCR repertoire. An alternative approach would be to transduce HSC with TCR genes. In vitro generation of mature, antigen-specific T cells by TCR gene transfer into thymus or cord-derived HSC has recently been reported. Allelic exclusion of the endogenous TCR β chain meant that mixed dimer formation was reduced, but not entirely avoided due to some endogenous α chain expression. However, while the risk of transformation of mature T cells is low, the risk in HSC may be higher, making this a less appealing strategy. In a clinical trial of X linked severe combined immunodeficiency disease, 4 children treated with HSC retrovirally transduced with the common γ chain developed T lymphoproliferative disorders. This was later found to be secondary to retroviral insertion into the LMO-2 oncogene intron on chromosome 11, with subsequent upregulation. Although there is no evidence to date of transformation of mature T cells with retroviral vectors, the use of lentiviral vectors is also being investigated, since it has been shown that lentiviral vectors insert near promoters at a lower frequency.
While there is a concern that low avidity, TAA specific CTL from the autologous repertoire may not be efficacious, high avidity, self-reactive CTL may pose the opposite problem. The majority of targets for tumor immunotherapy are over-expressed self proteins, and therefore there is a risk that targeting TAA may result in autoimmune damage. In murine models and in clinical trials it has been demonstrated that the successful induction of CTL responses against melanoma TAAs (such as melan A or gp100) has been associated with the development of vitiligo. T cell therapies targeting TAAs with a more ubiquitous distribution have not been studied in the same detail as yet, although it has been shown that high avidity p53 specific CTLs (generated in p53-/- transgenic mice) can provide tumor protection without causing autoimmune damage in mice. A moderately high affinity TCR was used in the TCR gene therapy trial, and work is now ongoing by the same group to test a higher avidity TCR. It remains to be seen whether any morbidity resulting from autoimmune disease outweighs the associated anti tumor benefit. A balance needs to be struck between TAA specific CTL which are of high enough avidity to mediate tumor killing, but which do not cause significant autoimmune damage to healthy tissue. It is likely that a large discrepancy between the expression level of the target antigen on tumor tissue compared to that on normal tissue will be an important factor in this regard, as will the pattern of distribution of the TAA in normal tissue.
Conclusion
Although TCR gene transfer holds promise, there may yet be obstacles to overcome with respect to either the safety or the efficacy of this strategy. While mispairing of endogenous and exogenous TCR chains may result in off target toxicity, high avidity CTL may cause on target toxicity by attacking normal tissues that express low levels of the target antigen. However, recent clinical trial data has demonstrated that TCR gene transfer is an effective means by which a defined population of antigen specific T cells can be generated which persist following adoptive transfer into patients. Research is ongoing to address the safety issues and to improve the expression of retrovirally introduced TCRs. Furthermore, while the adoptive transfer of antigen specific regulatory cells has been less well explored to date, this warrants further investigation as there are a number of potential clinical applications for such a strategy. Although unanswered questions remain, it is evident that TCR gene transfer holds clear promise for the treatment of malignancies and viral infections and may have potential to treat unwanted immunopathology in the future.
References
1. Stanislawski T, Voss RH, Lotz C, et al. Circumventing tolerance to a human MDM2-derived tumor antigen by TCR gene transfer. Nat Immunol. 2001;2:962-970.
2. Dembic Z, Haas W, Weiss S, et al. Transfer of specificity by murine alpha and beta T-cell receptor genes. Nature. 1986;320:232-238.
3. Clay TM, Custer MC, Sachs J, Hwu P, Rosenberg SA, Nishimura MI. Efficient transfer of a tumor antigen-reactive TCR to human peripheral blood lymphocytes confers anti-tumor reactivity. J Immunol. 1999;163:507-513.
4. Kessels HW, de Visser KE, Kruisbeek AM, Schumacher TN. Circumventing T-cell tolerance to tumour antigens. Biologicals. 2001;29:277-283.
5. Sadovnikova E, Jopling LA, Soo KS, Stauss HJ. Generation of human tumor-reactive cytotoxic T cells against peptides presented by non-self HLA class I molecules. Eur J Immunol. 1998;28:193-200.
6. Sadovnikova E, Stauss HJ. Peptide-specific cytotoxic T lymphocytes restricted by nonself major histocompatibility complex class I molecules: reagents for tumor immunotherapy. Proc Natl Acad Sci U S A. 1996;93:13114-13118.
7. Oka Y, Elisseeva OA, Tsuboi A, et al. Human cytotoxic T-lymphocyte responses specific for peptides of the wild-type Wilms' tumor gene (WT1 ) product. Immunogenetics. 2000;51:99-107.
8. Rubinstein MP, Kadima AN, Salem ML, et al. Transfer of TCR genes into mature T cells is accompanied by the maintenance of parental T cell avidity. J Immunol. 2003;170:1209-1217.
9. Dudley ME, Wunderlich JR, Robbins PF, et al. Cancer regression and autoimmunity in patients after clonal repopulation with antitumor lymphocytes. Science. 2002;298:850-854.
10. Gao L, Bellantuono I, Elsasser A, et al. Selective elimination of leukemic CD34(+) progenitor cells by cytotoxic T lymphocytes specific for WT1. Blood. 2000;95:2198-2203.
11. Xue SA, Gao L, Hart D, et al. Elimination of human leukemia cells in NOD/SCID mice by WT1-TCR gene-transduced human T cells. Blood. 2005;106:3062-3067.
12. Kessels HW, Wolkers MC, van DB, van d, V, Schumacher TN. Immunotherapy through TCR gene transfer. Nat Immunol. 2001;2: 957-961.
13. Morgan RA, Dudley ME, Wunderlich JR, et al. Cancer regression in patients after transfer of genetically engineered lymphocytes. Science. 2006;314:126-129.
14. Peggs KS, Verfuerth S, Pizzey A, et al. Adoptive cellular therapy for early cytomegalovirus infection after allogeneic stem-cell transplantation with virus-specific T-cell lines. Lancet. 2003;362:1375-1377.
15. Walter EA, Greenberg PD, Gilbert MJ, et al. Reconstitution of cellular immunity against cytomegalovirus in recipients of allogeneic bone marrow by transfer of T-cell clones from the donor. N Engl J Med. 1995;333:1038-1044.
16. Heslop HE, Ng CY, Li C, et al. Long-term restoration of immunity against Epstein-Barr virus infection by adoptive transfer of gene-modified virus-specific T lymphocytes. Nat Med. 1996;2:551-555.
17. Haque T, Wilkie GM, Taylor C, et al. Treatment of Epstein-Barr-virus-positive post-transplantation lymphoproliferative disease with partly HLA-matched allogeneic cytotoxic T cells. Lancet. 2002;360:436-442.
18. Szymczak AL, Workman CJ, Wang Y, et al. Correction of multi-gene deficiency in vivo using a single 'self-cleaving' 2A peptide-based retroviral vector. Nat Biotechnol. 2004;22:589-594.
19. Scholten KB, Kramer D, Kueter EW, et al. Codon modification of T cell receptors allows enhanced functional expression in transgenic human T cells. Clin Immunol. 2006;119:135-145.
20. Thomas S, Xue SA, Cesco-Gaspere M, et al. Targeting the Wilms tumor antigen 1 by TCR gene transfer: TCR variants improve tetramer binding but not the function of gene modified human T cells. J Immunol. 2007;179:5803-5810.
21. Hofmann M, Radsak M, Rechtsteiner G, et al. T cell avidity determines the level of CTL activation. Eur J Immunol. 2004;34:1798-1806.
22. Heemskerk MH, Hagedoorn RS, van der Hoorn MA, et al. Efficiency of T-cell receptor expression in dual-specific T cells is controlled by the intrinsic qualities of the TCR chains within the TCR-CD3 complex. Blood. 2007;109:235-243.
23. Cohen CJ, Zhao Y, Zheng Z, Rosenberg SA, Morgan RA. Enhanced Antitumor Activity of Murine-Human Hybrid T-Cell Receptor (TCR) in Human Lymphocytes Is Associated with Improved Pairing and TCR/CD3 Stability. Cancer Res. 2006;66:8878-8886.
24. Hart DP, Xue SA, Thomas S, et al. Retroviral transfer of a dominant TCR prevents surface expression of a large proportion of the endogenous TCR repertoire in human T cells. Gene Ther. 2008;15:625-631.
25. Sebestyen Z, Schooten E, Sals T, et al. Human TCR That Incorporate CD3{zeta} Induce Highly Preferred Pairing between TCR{alpha} and {beta} Chains following Gene Transfer. J Immunol. 2008;180:7736-7746.
26. Van der Veken, LT, Hagedoorn RS, van Loenen MM, Willemze R, Falkenburg JH, Heemskerk MH. Alphabeta T-cell receptor engineered gammadelta T cells mediate effective antileukemic reactivity. Cancer Res. 2006;66:3331-3337.
27. Heemskerk MH, Hoogeboom M, Hagedoorn R, Kester MG, Willemze R, Falkenburg JH. Reprogramming of virus-specific T cells into leukemia-reactive T cells using T cell receptor gene transfer. J Exp Med. 2004;199:885-894.
28. van Lent AU, Nagasawa M, van Loenen MM, et al. Functional human antigen-specific T cells produced in vitro using retroviral T cell receptor transfer into hematopoietic progenitors. J Immunol. 2007;179:4959-4968.
29. Zhao Y, Parkhurst MR, Zheng Z, et al. Extrathymic generation of tumor-specific T cells from genetically engineered human hematopoietic stem cells via Notch signaling. Cancer Res. 2007;67:2425-2429.
30. Recchia A, Bonini C, Magnani Z, et al. Retroviral vector integration deregulates gene expression but has no consequence on the biology and function of transplanted T cells. Proc Natl Acad Sci U S A. 2006;103:1457-1462.
31. Hacein-Bey-Abina S, von KC, Schmidt M, et al. A serious adverse event after successful gene therapy for X-linked severe combined immunodeficiency. N Engl J Med. 2003;348:255-256.
32. Marshall E. Gene therapy. Second child in French trial is found to have leukemia. Science. 2003;299:320.
33. Check E. Gene therapy put on hold as third child develops cancer. Nature. 2005;433:561.
34. Yee C, Thompson JA, Roche P, et al. Melanocyte destruction after antigen-specific immunotherapy of melanoma: direct evidence of t cell-mediated vitiligo. J Exp Med. 2000;192:1637-1644.
35. Vierboom MP, Nijman HW, Offringa R, et al. Tumor eradication by wild-type p53-specific cytotoxic T lymphocytes. J Exp Med. 1997;186:695-704.
36. Spiotto MT, Fu YX, Schreiber H. Tumor immunity meets autoimmunity: antigen levels and dendritic cell maturation. Curr Opin Immunol. 2003;15:725-730.
Accepted 10 November 2008
Published 27 November 2008


