Therapeutic potential of mouse bone marrow mesenchymal stromal cells transplantation in ameliorating of CCL4-induced liver damage (in vivo study)
Dima Joujeh1, Abduljalil Ghrewaty1, Chadi Soukkarieh2, Adnan Almarrawi1, Jamal Abdul Naser Darwicha3
1 Department of Biotechnology Engineering, Faculty of Technical Engineering, University of Aleppo, Syria
2 Department of Animal Biology, Faculty of Sciences, Damascus University, Damascus, Syria
3 Department of Pharmacology and Toxicology, Faculty of Pharmacy, Arab International University, Syria
Correspondence:
Dr. Dima Joujeh, Department of Biotechnology Engineering, Faculty of Technical Engineering, University of Aleppo, Syria
Phone: (+963) 994-046-745
E-mail: dimajoujeh@gmail.com
Citation: Joujeh D, Ghrewaty A, Soukkarieh C et al. Therapeutic potential of mouse bone marrow mesenchymal stromal cells transplantation in ameliorating of CCL4-induced liver damage (in vivo study). Cell Ther Transplant 2022; 11(1): 58-68.
Accepted 28 January 2022
Summary
Liver diseases pose a major global health problem. In this study, the effect of bone marrow derived mesenchymal stromal cells MSC(M) in liver damage induced by CCl4 treatment was investigated.
Materials and methods
Balb/c mice were injected by (1 ml/kg body weight) of CCl4 twice a week for 7 weeks. The mice were then intravenously injected with MSC(M) (at the passage 0), or physiological saline (PBS, control group). Four weeks after transplantation, serum levels of ALT, AST, ALP and albumin were measured, liver histopathology was performed, and ELISA technique was carried out to detect the serum levels of IL-4 and IFN-γ.
Results
As compared with PBS-treated animals, MSC(M)- treated group presented with lower levels of ALT and ALP, being also associated with less pronounced changes in serum albumin. Histological study was consistent with biochemical data, suggesting an improvement in MSC(M)-treated group compared with PBS group. Transplantation of MSC(M) increased production of IL-4 and IFN-γ compared to PBS group.
Conclusion
Our results demonstrated that MSC(M) transplantation could facilitate recovery from chemically induced liver damage. Therefore, MSC(M) transplantation may represent a new concept for the treatment of liver diseases.
Keywords
Mice, liver damage, CCl4, bone marrow stromal cells, mesenchymal, cell transplantation.
Introduction
Although the liver has a considerable inherent regenerative capacity, a sufficient and prolonged may result into liver damage and onset of hepatic fibrosis [1]. For severe hepatic diseases, liver transplantation is one of the more effective treatments [2]. However, the tremendous gap between offered donor organs and those required for transplantation is the major limitation of liver replacement therapy [3]. High cost and transplant rejection following liver transplantation, have also largely limited its clinical application [4]. Therefore, alternative or adjuvant therapies are urgently needed [3].
Recently, regenerative medicine using different stem cells has been considered an attractive therapy for treating patients with severe liver disease [5], since these cells have the ability of self-renewal and maturation [6]. Stem cells are defined as undifferentiated cells from an embryo, fetus or an adult, which have the potential to produce various differentiated tissue cells under appropriate stimuli [5]. Bone marrow (BM) provides a more readily available source of cells [7]. Bone marrow cells are presently considered to be the most promising cell source for the cell therapy of various diseases [8]. Mesenchymal stromal cells (MSCs) have been documented as a promising technique for cell therapy and have been successfully applied in the treatment of various diseases [3]. Multipotent MSCs represent a remarkable stem cell population for application in liver-directed cell transplantation, since they are readily obtained from bone marrow aspirates and can be expanded in culture [9], through as many as 50 population doublings in about 10 weeks [10], thus producing a large number of potent cells [9]. In addition, BM-MSCs possess many advantages such as autologous sources, abundance of cells, an immune-modulatory capacity, secretion of cytokines and growth factors, homing to injury sites, and hepatic differentiation [11].
The present study aimed to investigate the therapeutic effect of bone marrow-derived mesenchymal stromal cells MSC(M) transplantation in alleviation of CCl4-induced liver damage in mice.
Materials and methods
Experimental Animals
Healthy male mice (Balb/c, 4-6 weeks) were used in this study. Mice were housed in clean cages of 65×25×15 cm containing woodchip bedding. Mice were housed in a temperature (temperature 24±2°C) and light-controlled room (12h light/dark cycle), with free access to food and water. The animals were left for two weeks to acclimatize to their surroundings before starting the experiment. All procedures were performed according to the Guide for the Care and Use of Laboratory Animals and the ethical standards of our institution.
Liver damage induction and MSC(M) preparation
To establish the liver-injury mice model, male Balb/c mice were intraperitoneally injected with (1 ml/kg body weight) of CCl4 dissolved in olive oil twice a week for 7 consecutive weeks.
In the current study, 4-6 weeks male healthy BALB/c mice were used as donors of MSC(M). Mice were sacrificed by cervical dislocation. MSC(M) were flushed from the medullary cavities of the tibia and femur using a needle with complete media (Dulbecco’s modified Eagle’s medium (DMEM) (Euroclone, Italy). The cells were grown in (4-5 ml) of DMEM medium supplemented with (20% FBS, 1% L-glutamine, 1% penicillin/streptomycin and 1.5 µg/ml amphotericin B) (Euroclone, Italy), in a 25 cm2 culture flask, and incubated at 37°C with 5% CO2. 24 h later, the culture medium was replaced to remove non-adherent cells and tissue debris. MSC(M) at passage 0 (P0) were used for transplantation.
Experimental Protocol
The mice were divided into the following groups:
• Control group (Group I): This group included healthy normal mice, which were not exposed and did not receive any treatment.
• Experimental group: mice were intraperitoneally injected with CCl4 (1 ml/kg body weight) of dissolved in olive oil twice a week for 7 consecutive weeks. After the last injection of CCl4, three mice were randomly selected from this group, blood samples were collected and serum ALT level was determined to ensure that liver damage had been induced before continuing the experiment. Mice in this group were randomly divided into two groups, as follows:
• PBS-treated group (Group II): mice were intravenously injected into the tail vein with 0.5 ml of phosphate buffer saline (PBS 1X).
• MSC(M) treated group (Group III): mice were intravenously injected with MSC(M). MSC(M) were washed with PBS (1X) and trypsinized with 0.25% trypsin, then (approximately 3×106 of MSC(M) per mouse) were re-suspended in (0.5 ml) of PBS and injected into the tail vein.
The mice from all studied groups (I, II, III) were sacrificed 4 weeks after transplantation. Venous blood and liver tissue samples were collected for further analyses. At the end of the experiment, the body weight and liver weight of the animals in all studied groups were determined. The liver to body weights ratio was determined as follows:
Liver to body Ratio = (liver weight (g)/(mouse body weight (g)-liver weight (g))) *100.
Laboratory analyses
Venous blood was collected, and blood samples were centrifuged at 3000 rpm for 5 minutes. Serum samples were subsequently analyzed to evaluate the activities of alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (ALP), and albumin.
Liver histology was performed to assess liver damage 4 weeks after MSC(M) transplantation. For light microscopic examination, the liver from each animal was carefully dissected and the specimens were fixed in 10% formalin for 48 hours. Paraffin sections were prepared and stained with hematoxylin and eosin (H&E) to display the histological details. Histological damage was evaluated by a pathologist who was blinded to the experimental groups.
At the end of the experiment, blood samples were collected and centrifuged at 3000 rpm for 5 min. The serum levels of interleukin-4 (IL-4) and IFN-γ cytokines were measured by ELISA assay kits according to the manufacturer’s instructions (Sun Red, China).
Results
The cultured MSCs were injected into syngeneic mice treated with hepatotoxic agent CCl4.
The results of this study showed remarkable significant increase in the liver weight and the liver weight to body weight ratio in PBS group compared with the normal control group. MSC(M) transplantation alleviated the increase in the liver weight and even decreased the ratio to a level closer to that of normal mice. There was no significant difference in the ratio between the MSC(M) treated group and the normal control group (Table 1).
Table 1. Body mass, liver weight and liver-to-body weight ratios of all studied groups
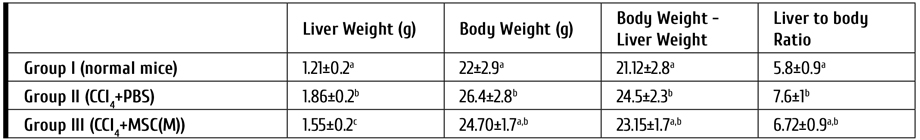
Note: All values are represented as mean ± SD. Mean values with different letters over the same column are significantly different at (P<0.05)
Serum levels of ALT, AST, ALP, and albumin were evaluated. After intraperitoneal injection of CCl4 for consecutive 7 weeks, serum levels of ALT were markedly increased in the experimental group (120±5.3), as compared to control group. PBS group exhibited markedly increased serum levels of ALT and ALP compared with control normal mice. The levels of ALT and ALP in the MSC(M)-treated group were significantly reduced compared to the PBS group being close to the normal control group. In addition, there was a significant decrease in serum levels of albumin in PBS group when compared with the control group. Significantly increased serum albumin levels were noticed in MSC(M)-treated group when compared to the PBS group. The levels of these parameters in control and MSC(M) treated group did not show any significant differences. Nearly similar AST levels were observed in MSC(M) and PBS groups (Table 2).
Table 2. Serum levels of ALT, AST, ALP, and albumin in the studied groups

Note: All values are represented as mean ± SD. Mean values marked with different letters (a,b) over the same column are significantly different at (P<0.05)
Histopathological analysis of liver sections
The liver of the control group was reddish-brown, with smooth and glossy surface. The liver of the PBS group was pale-brown, overtly swollen with coarse surface and necrotic spots. In MSC(M)-treated group, the liver surface was slightly coarse, less swollen, more reddish, and glossy compared with livers from the PBS group. Necrotic spots on the surface were noticeably reduced (Fig. 1).

Figure 1. Morphologic examination of the livers of the study groups. (A). The liver of the normal control group was smooth, lustrous, and reddish. (B) In the PBS group, the liver was pale-brown with coarse surface and overtly swollen. (C) In the mice receiving MSC(M) transplantation, the liver surface was slightly coarse, less swollen, more reddish, and lustrous than those of PBS group
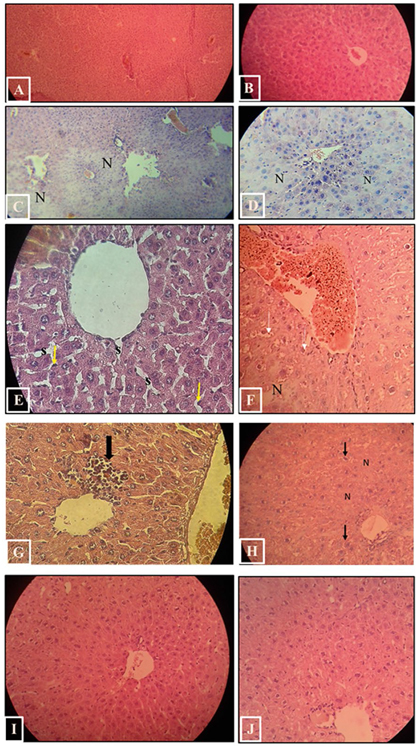
Figure 2. H&E-stained sections in Balb/c mice’s liver of the study groups. A, B. Control group. C–H. PBS group. C-D. Marked damage with disorganization of hepatic architecture, hepatocytes necrosis (N) can be seen. E. The blood sinusoids (s) are dilated and surrounded by Kupffer cells (arrows) with prominent nuclei. F. Vascular dilatation and congestion can be seen, some hepatocytes showed vacuolated cytoplasm (arrows). G. Inflammatory cell infiltration (arrow). H. hepatocytes with vacuolated cytoplasm (arrows). I, J. MSC(M) treated group. nearly normal organization of hepatic lobules. Hepatocytes appeared nearly similar to that of the control mice
Light microscope examination of normal liver tissue sections (control group) showed classical hepatic architecture (Fig. 2. A,B). Hepatocytes are arranged in cords that radiate from the central veins and separated by blood sinusoids. They had rounded nuclei and well-preserved cytoplasm. Some hepatocytes were binucleated. Blood sinusoids are lined by Kupffer cells and endothelial cells. Normal blood vessels and bile ducts were observed in Portal areas. PBS group showed marked affection with disorganization of hepatic architecture. Cellular necrosis was observed. Some hepatocytes appeared swollen with extensively vacuolated cytoplasm. Liver sections also revealed vascular dilatation and congestion in the portal areas and in the central veins. Some parts showed dilated blood sinusoids, which were lined by many Kupffer cells with prominent nuclei. Inflammatory cell infiltration was also detected (Fig. 2. C-H). The histopathological lesions were effectively attenuated to varying extents, in the MSC(M) treated group. Examination of H&E-stained sections showed nearly normal organization of hepatic lobules. A marked reduction of cellular necrosis was observed (Fig. 2, I, J). Hepatocytes appeared nearly similar to that of the control mice. Most hepatocytes had rounded nuclei and well-preserved cytoplasm, they were arranged around slightly dilated and congested central veins and separated by hepatic blood sinusoids. Few hepatocytes appeared with vacuolated cytoplasm. Liver sections demonstrated slight inflammatory cell infiltration. Portal areas appeared nearly normal with slightly congested blood vessels.
Serum Interleukin-4 (IL-4) and Interferon-γ (IFN-γ) Levels
To determine if MSC(M) transplantation affects the cytokine release, the serum levels of IL-4 and IFN-γ were measured by ELISA. As shown in Fig. 3, IL-4 level declined in the PBS group compared to the control group, and this effect was blocked by MSC(M) transfusion. Serum IL-4 level was elevated in MSC(M) treated group, as compared with the PBS group. Serum IFN-γ level was elevated in PBS group compared with the control group. The secretion of IFN-γ was higher in the MSC(M) treated group than in the control group and PBS group, at one month post transplantation.

Figure 3. Serum levels of IL-4, and IFN-γ cytokines. Sera were collected one month after MSC(M) transplantation, and cytokines were measured with enzyme-linked immunosorbent assay (ELISA). After MSC(M) transplantation, the IL-4, and IFN-γ levels were increased compared to PBS group
Discussion
Liver disease causes approximately two million deaths annually worldwide [12]. Therefore, there is an urgent need to develop new techniques to stimulate liver regeneration. In this regard, the potential of MSC therapy is of great interest in regard of liver regeneration [13]. Cell transplantation programs may provide a hopeful technology to replace organ transplantation [3].
Since CCl4 is toxic and may cause death, establishment of liver damage model in mouse is challenging [14]. When metabolized in liver by the cytochrome P450 monooxygenases, CCl4 produces free oxygen species [15, 16]. CCl4 activation to trichloromethyl and trichloromethyl peroxy radicals is stimulates lipid peroxidation and protein oxidation in the liver, causing membrane damage and liver injury [17].
Bone marrow mesenchymal stromal cells were isolated, cultured, and characterized in our previous study (data not shown). Although the isolated cells showed the characteristics of mesenchymal stromal cells, we guess that the population also contained a low proportion of hematopoietic stem cells, since we used the cells at the zero passage (P0), since hematopoietic stem cells have been reported to exist in MSC cultures even after nine in vitro passages [18].
In the current study, MSC(M) at passage 0 were used for transplantation, thus being different from the earlier experiments with MSC(M) therapy published so far, where MSC(M) were mostly injected at passage 3 (P3 MSC(M)).
The in vitro expansion is always required for MSC-based therapies in order to generate sufficient MSC(M) numbers for transplantation. Clinical recommendations for medical MSC usage usually apply cells from 3-5 passages. However, unexpected risks may occur during cell growth, including lack of phenotype, contamination and reduction in efficacy, possibly leading to therapy failure. It has also been reported that additional expansion might attenuate the stemness property of MSCs, thus contributing to reduction of therapeutic potential [19].
Previous report demonstrated that human MSCs subjected to extensive passaging may undergo morphological, phenotypic, and genetic changes [20]. It has been shown that the monolayer cultures significantly affect cell behavior, e.g., leading to cell senescence and impairment of multi-potency [19].
We have also studied the effects of MSC(M) transplantation upon body weight and liver weight. CCl4 is known to be a potent toxicant associated with the liver damage [21]. Determination of the liver weight to body weight ratio of mice may reflect structural and functional changes of the liver after CCl4 injury [22]. Since the body mass measures include the liver weight, it was subtracted from body weight to obtain a "liver-free" estimate of the body weight. Subtraction the liver weight is necessary because otherwise the measurable body weight will always reflect changes in the liver weight. It may make little difference in practice, because the liver weight is small, as compared with total body weight [23]. Significant increase in the liver weight was observed in PBS group compared with control group. This elevation in liver weight after CCl4 intoxication has been well supported by previous research [21, 24]. However, MSC(M) treatment seems to significantly reduce liver inflammation and hence, the liver weight. The ratio of liver weight to body mass was higher in PBS group with significant difference compared to the normal control group. MSC(M) treatment caused a non-significant decrease in this ratio compared to the PBS-treated group, but it became closer to the values of normal control group.
Estimation of biochemical indexes is widely accepted as a biomarker of liver damage [25]. Enzymes represent sensitive metabolic markers, thus even slight changes in enzyme activities would affect the organism [26]. Serum ALT level is usually elevated in case of serious liver damage and the extent of organ damage depends on the type of toxin, its mechanism of action and duration of exposure [26]. Serum ALT activity is a reliable and sensitive marker of liver disease [27].
The present study revealed a marked increase in the level of ALT upon exposure to CCl4 for 7 weeks (experimental group), which indicates considerable hepatocellular injury [28].
Exposure to CCl4 leads to liver injury [15]. Oxidative stress is considered to be the major pathogenic process of CCl4-induced liver injury [29]. This process causes changes in the of cell membrane permeability [15]. As a result, cytoplasmic ALT can leak into the bloodstream, and serum ALT level is increased [29], and can be determined [30]. In this study, we did not use liver toxin after transplantation of MSC(M). During treatment, it is important to eliminate the pathogen, in order to treat the disease efficiently without causing unnecessary complications. Such a strategy has the advantage of enhancing the recipient’s therapy regimen [31].
The results showed a decrease in ALT level in the PBS group compared to experimental group, which is explained by self-recovery and regeneration of mouse livers after CCl4 injection was discontinued. However, alleviation of liver damage occurred significantly faster in mice treated with MSC(M) than in untreated mice. MSC(M)-treated mice showed statistically significant improvement when compared to the PBS-treated group. These results reflect the important role of MSC(M) and show that MSC(M) transplantation can enhance regenerative capacity of the liver and improve affected tissues.
Alkaline phosphatase activity is a very useful serum biochemical marker of liver disease [32]. The present study revealed a significant increase in ALP level of PBS-treated group compared with MSC(M)-treated group. Liver ALP is synthesized by the bile duct. Previously, ALP was thought to be increased, due to inability of liver cells to release the enzyme with bile. It is, however, accepted that ALP activity is increased due to higher enzyme synthesis [33], with involvement of biliary ways [34]. The increased hepatic enzyme activity clearly parallels the rise in serum alkaline phosphatase activity, which is primarily caused by increased ALP mRNA translation (mediated by elevated bile acid concentration), and increased secretion of ALP into serum via canalicular leakage into the hepatic sinusoids by still unclear mechanisms [35].
Albumin synthesis is highly sensitive to CCl4 effects [36]. Albumin and other hepatic secretory proteins are synthesized by polysomes bound to the endoplasmic reticulum. CCl4 causes damage to hepatocytes, including disruption of hepatic cells with polysome disaggregation and decrease in protein synthesis [37].
On the other hand, it was thought that CCl4 toxicity leads to damage of Golgi apparatus, which, in turn, negatively affects protein packaging and release from hepatocytes [36]. One month after MSC(M) transplantation, liver injury markers (ALT and ALP) showed positive changes compared with PBS group. A significant increase in serum albumin level was noticed in MSC(M)-treated group compared to the PBS group, which suggests that transplantation of MSC(M) results in significant restoration of specific liver function.
The liver histology studies were consistent with biochemical results, suggesting an improvement in MSC(M) treated group compared with PBS group. In the current study, CCl4 intoxication resulted in disorganization of hepatic architecture, necrosis of hepatocytes, cytoplasm vacuolation, vascular congestion and dilation, dilatation of sinusoids and infiltration with inflammatory cell, as revealed by light microscope examination of livers from PBS group. Carbon tetrachloride is metabolized by cytochrome to reactive oxygen species, resulting in membrane lipid peroxidation and oxidative stress injury, and, finally, hepatocyte necrosis and dysfunction [38]. Necrosis is viewed as a largely unregulated sequence of physicochemical stress, characterized by mitochondrial impairment, adenosine triphosphate (ATP) depletion, and subsequent failure of ATP-dependent ion pumps. These changes result in rapid swelling of cells and cell organelles ("oncosis") accompanied by the formation of membrane "blebs" and eventual cell rupture [39].
Microscopical examination of liver sections in PBS group showed vascular dilatation and congestion. Dilatation may be caused by increase levels of prostaglandin synthesis that leads to smooth muscle relaxation and vasodilatation [40]. The congestion may be due to fluid loss from the dilated vessels, so they become filled with red blood cells [40]. This congestion, as suggested by Hong et al., (1991) and Wijetunga et al., (2003), is a typical early index of hepatotoxicity [17]. The liver sections of PBS group exhibited cytoplasmic vacuolation and increase in cell volume which are due to the loss of the cell's regulating mechanism for pumping out water from the inside. Cell swelling in CCl4 intoxication is due to altered cell membrane permeability. CCl4 is a non-polar lipophilic substance, thus leading to changes in the physical and chemical properties of both cytoplasmic and mitochondrial lipid membranes, and resulting in disruption of Na+/K+ pump and migration of interstitial fluids to the hepatocytes [40].
After MSC(M) transplantation, marked reduction in liver damage was observed, as compared to PBS group, thus suggesting heterogeneous response to cell therapy in distinct animals. Microscopic examination showed improvement in the histopathological changes induced by CCl4, and in hepatic lobular architecture. Previous study has shown that MSCs secrete several factors, i.e., nitric oxide and prostaglandin E2, which enhance antioxidant protection, inhibit oxidative factors, and reduce the hepatocyte necrosis [11]. However, the mechanism by which MSC(M) repair liver damage remain unclear [41].
The studies of IL4 and IFN-γ serum levels by ELISA have shown some differences in IL-4 between CCl4-treated animals and controls. Cytokines are a class of polypeptide micro-molecules secreted by various cells, which are able to regulate cell growth and differentiation, immune function, inflammation and wound healing [15]. E.g., interferon-γ (IFN-γ) is the hallmark cytokine of T helper 1 (Th1) cells, whereas interleukin 4 (IL-4) has the same role in Th2 cells [42]. The results showed that the serum level of IL-4 decreased in PBS treated mice compared to the control group (intact mice). After MSC(M) transplantation, the IL-4 level increased.
Differences in IL-4 levels between serum of mice treated and those not treated with MSC(M) proved that MSC(M) had a therapeutic effect. IL-4 is one of the widely recognized immune regulatory cytokines capable of suppressing inflammation [43]. It has been used successfully in the treatment of inflammatory diseases in animal models, and in experimental studies, IL-4 injections significantly improved the condition of psoriatic dermatitis [44]. Several studies suggest that treatments that act to increase the concentration of interleukin-4 in tissues may be beneficial in treating inflammation [45, 46].
However, the exact mechanisms by which IL-4 exerts its anti-inflammatory effects are not well understood [44]. The lower levels of the anti-inflammatory cytokine IL-4 found in the injured group compared to control is in accordance with previous studies showing suppression of this cytokine during acute injury [47-49].
Our results are consistent with prior studies that showed that the IL-4 level was higher in the MSC-treated group compared to the untreated mice [43, 49, 50]. It has been demonstrated that MSCs caused the TH2 cells to increase secretion of IL-4 [51, 52]. Chai et al., (2016) have shown that MSC(M) may increase IL-4 secretion in rats with liver fibrosis induced by dimethyl nitrosamine (DMN) both in vitro and in vivo [49]. Jia et al., (2018) indicated that the IL-4 mRNA expression was significantly higher in corneal grafts from MSCs-treated groups when compared with controls (PBS group) [50]. Our data showed that anti-inflammatory cytokine IL-4 exhibited remarkable increase in the MSC(M)-treated group. These findings may explain how MSC(M) mediate the cell repair in the damaged liver which could be partially associated with increased IL-4 production.
IFN-γ is an important Th1 cytokine [48]. It is produced predominantly by natural killer and Th1 cells, regulates their activity, and is critical for innate and adaptive immunity [47]. Our results demonstrated that serum IFN-γ level increased after CCl4-induced liver injury (PBS group) compared to the control group. Our results are consistent with previous studies showing that CCl4 injury caused elevation of serum IFN-γ levels [22, 53]. Previous study demonstrated that CCl4 injection into mice activated type 1 innate lymphoid cells (ILC1s), which, in turn, produced IFN- γ and protected mice from CCl4-induced acute liver injury. IFN-γ released from activated ILC1s promoted survival of the hepatocytes via upregulation of Bcl-xL [53]. Interestingly, IFN-γ followed the trend of the Th2 cytokine (IL-4), since its level increased after intravenous infusion of MSC(M). One may propose more than one explanation for this finding.
In the current study, experimental animals received syngeneic MSC(M) without prior immunosuppression with cyclosporine. Syngeneic transplantation is still believed to be the safest way of MSCs administration and does not cause any immune reaction [54]. It is possible that the immune system responds to infused MSC(M) as the cells are produced in culture and differ in size and protein expression patterns from the non-cultured MSC(M). Moreover, only low numbers of mesenchymal stromal cells are normally present in the circulation. Meanwhile, higher MSC numbers are present after MSC(M) infusion, thus, probably, activating the response. It is thus likely that the immune reaction induced after MSCs transplantation represented a response to cells perceived as foreign objects and/or presented at an unusual location, rather than a MSC-specific response [55].
It has also been reported that Th1 cytokines are involved into the graft rejection [56]. A previous work indicated that this cytokine may be a useful predictor of acute graft-versus-host disease (GvHD) [57]. Some murine studies reported high serum IFN- levels in acute GvHD [57-59]. Our in vivo study demonstrated that syngeneic MSCs are not fully immuneprivileged. Along with their therapeutic effects, they cause an immune response and may be rejected. The transplanted cells may become immunogenic during extracorporeal manipulations, despite identical genotypes of donor and recipient. It has been shown that the in vitro cultures of cells may alter their phenotype through epigenetic changes [54]. The opinion that syngeneic transplantation is safe comes from organ and tissue transplantology, where the biological material is transferred without any additional in vitro processing which is not the case in majority of experimental MSC transplants [54]. The strategies that reduce MSC immunogenicity can potentially prolong their in vivo persistence and improve the therapeutic effects. Thus, the modulation of immune responses is a prerequisite for preclinical and clinical studies in MSC therapy.
On the other hand, MSC-mediated immunosuppression was also reported to depend on prior activation by pro-inflammatory cytokines [60]. Previous studies also suggested that the immunosuppressive ability of MSC(M) require preliminary activation by IFN-γ alone, or in combination with other chemokines [61]. However, once MSC is activated, they can release several soluble factors, such as prostaglandin E2 (PGE2), inducible nitric-oxide synthase (iNOS), indoleamine 2,3-deoxigenase (IDO), and IL-6 that exert immunomodulatory effects on other cell types [60]. Therefore, elevated IFN-γ in the MSC(M) group may play a role in the immunomodulatory properties of MSC(M) [61]. Expression of IDO and other anti-inflammatory factors by MSCs is strongly stimulated under inflammatory conditions, suggesting that the immunomodulatory effects of MSCs act as a feedback mechanism to control ongoing immune responses [55]. However, further studies are required in order to elucidate the mechanism of immune response upon intravenous injection of syngeneic MSC(M).
Our results demonstrated that MSC(M) transplantation could facilitate recovery from chemically induced liver damage. Several mechanisms could explain the therapeutic effects of MSC(M) in liver injury [62], as follows: 1) potential migration of MSC(M) to damaged liver with possible differentiation into hepatocytes and promoted recovery from chemically induced liver damage [15]; 2) secretion of paracrine factors such as cytokines, hormones and growth factors, thus promoting tissue repair; 3) transfer of organelles (e.g., mitochondria) and/or molecules through tunneling nanotubes. 4) MSC-mediated transfer of proteins/peptides, hormones, RNA, and/or chemicals by extracellular vesicles, such as exosomes or microvesicles [63]. The contribution of paracrine effects has been further supported by recent studies reporting the therapeutic benefit of MSC-derived biomolecules for treatment of acute liver injury [62].
Conclusion
We presented that transplantation of MSC(M) could successfully promote liver regeneration and ameliorate CCl4-induced liver damage, but elicits an immune response upon intravenous injection in murine model. However, further investigations are needed to increase the reliability of the clinical efficacy of MSC(M), to evaluate safety of MSC(M) therapy, as well as clarify the exact therapeutic mechanism of MSC(M), determine optimal injection route, timing and dosage of MSC administration, optimal stem cell source, and, possibly, to develop therapeutic strategies aiming for improved effectiveness of MSC(M) transplantation. We hope that our findings will contribute to the improvement of MSC(M)-based therapies for liver disease.
Conflicts of interest
None declared.
References
-
Eom Y, Shim K, Baik S. Mesenchymal stem cell therapy for liver fibrosis. Korean J Intern Med. 2014; 30, 580-589.
doi: 10.3904/kjim.2015.30.5.580 - Chang Y, Liu J, Lin P, Sun L, Peng C, Luo G, Chen T, Lee R, Lin S, Harn H, Chiou T. Mesenchymal stem cells facilitate recovery from chemically induced liver damage and decrease liver fibrosis. Life Sciences, 85, 517-525 (2009). doi: 10.1016/j.lfs.2009.08.003
- Hegab M, Abd-Allah S, Badawey M, Saleh A, Metwally A, Fathy G, Nada S, Abdel-Rahman S, Saleh A, Fawzy A, Abu El-Magd M. Therapeutic potential effect of bone marrow-derived mesenchymal stem cells on chronic liver disease in murine Schistosomiasis Mansoni. J Parasit Dis, 42(2), 277-286 (2018). doi: 10.1007/s12639-018-0997-8
- Hao T, Chen J, Zhi S, Zhang Q, Chen G, Yu F. Comparison of bone marrow-vs. adipose tissue-derived mesenchymal stem cells for attenuating liver fibrosis. Exp Ther Med. 2017 Dec;14(6):5956-5964. doi: 10.3892/etm.2017.5333
- Haraguchi T, Tani K, Takagishi R, Oda Y, Itamoto K, Yamamoto N, Terai S, Sakaida I, Nakazawa H, Taura Y. Therapeutic potential of canine bone marrow stromal cells (BMSCs) in the carbon tetrachloride (CCl4) induced chronic liver dysfunction mouse model. J Vet Med Sci. 2012 May;74(5): 607-611. doi: 10.1292/jvms.11-0505
- Farouk S, Sabet S, Abu Zahra FA, El-Ghor AA. Bone marrow derived-mesenchymal stem cells downregulate IL17A dependent IL6/STAT3 signaling pathway in CCl4-induced rat liver fibrosis. PLoS One. 2018 Oct 22;13(10):e0206130.
doi: 10.1371/journal.pone.0206130 - Buck NE, Cheah DM, Elwood NJ, Wright PF, Allen KJ. Correction of copper metabolism is not sustained long term in Wilson's disease mice post bone marrow transplantation. Hepatol Int. 2008;2(1):72-79. doi: 10.1007/s12072-007-9039-9
- Oyagi S, Hirose M, Kojima M, Okuyama M, Kawase M, Nakamura T, Ohgushi H, Yagi K. Therapeutic effect of transplanting HGF-treated bone marrow mesenchymal cells into CCl4-injured rats. J Hepatol. 2006 Apr;44(4):742-748. doi: 10.1016/j.jhep.2005.10.026
- Popp FC, Slowik P, Eggenhofer E, Renner P, Lang SA, Stoeltzing O, Geissler EK, Piso P, Schlitt HJ, Dahlke MH. No contribution of multipotent mesenchymal stromal cells to liver regeneration in a rat model of prolonged hepatic injury. Stem Cells. 2007 Mar;25(3):639-645. doi: 10.1634/stemcells.2006-0515
- Abdel Aziz MT, Atta HM, Mahfouz S, Fouad HH, Roshdy NK, Ahmed HH, Rashed LA, Sabry D, Hassouna AA, Hasan NM. Therapeutic potential of bone marrow-derived mesenchymal stem cells on experimental liver fibrosis. Clin Biochem. 2007 Aug;40(12):893-899. doi: 10.1016/j.clinbiochem.2007.04.017
- Truong NH, Nguyen NH, Le TV, Vu NB, Huynh N, Nguyen TV, Le HM, Phan NK, Pham PV. Comparison of the treatment efficiency of bone marrow-derived mesenchymal stem cell transplantation via tail and portal veins in CCl4-Induced mouse liver fibrosis. Stem Cells Int. 2016;2016: 5720413. doi: 10.1155/2016/5720413
- Asrani SK, Devarbhavi H, Eaton J, Kamath PS. Burden of liver diseases in the world. J Hepatol. 2019 Jan;70(1):151-171.
doi: 10.1016/j.jhep.2018.09.014 - Margini C, Vukotic R, Brodosi L, Bernardi M, Andreone P. Bone marrow derived stem cells for the treatment of end-stage liver disease. World J Gastroenterol. 2014;20(27):9098-9105. doi: 10.3748/wjg.v20.i27.9098
- Truong H, Nguyen H, Nguyen T, Le, Tran HG, Huynh N, Nguyen TV. Establishment of a standardized mouse model of hepatic fibrosis for biomedical research. Biomed Res Ther. 2014); 1, 9. doi: 10.7603/s40730-014-0009-2
- Wang M, Zhang X, Xiong XI, Yang Z, Li P, Wang J, Sun YU, Yang Z, Hoffman RM. Bone marrow mesenchymal stem cells reverse liver damage in a carbon tetrachloride-induced mouse model of chronic liver injury. In Vivo. 2016 May-Jun;30(3):187-193. PMID: 27107074
- Scholten D, Trebicka J, Liedtke C, Weiskirchen R. The carbon tetrachloride model in mice. Lab Anim. 2015; 49(1 Suppl):4-11.
doi: 10.1177/0023677215571192 - Adekomi DA, Oyesomi TO, Ajao MS, Ojo OA, Onikanni SA. Impact of liver damage on the histoarchitectural profile of the cerebellar cortex in rats. African J. Cell. Pathol. 2013. 1(1): 1-8. doi: 10.5897/AJCPATH13.005
- Zhu H, Guo ZK, Jiang XX, Li H, Wang XY, Yao HY, Zhang Y, Mao N. A protocol for isolation and culture of mesenchymal stem cells from mouse compact bone. Nat Protoc. 2010; 5(3):550-560. doi: 10.1038/nprot.2009.238
- Jiang T, Xu G, Wang Q, Yang L, Zheng L, Zhao J, Zhang X. In vitro expansion impaired the stemness of early passage mesenchymal stem cells for treatment of cartilage defects. Cell Death Dis. 8 (2017). doi: 10.1038/cddis.2017.215
- Yang YK, Ogando CR, Wang See C, Chang TY, Barabino GA. Changes in phenotype and differentiation potential of human mesenchymal stem cells aging in vitro. Stem Cell Res Ther. 2018; 9(1):131. doi: 10.1186/s13287-018-0876-3
- Ullah H, Khan A, Baig MW, Ullah N, Ahmed N, Tipu MK, Ali H, Khan S. Poncirin attenuates CCL4-induced liver injury through inhibition of oxidative stress and inflammatory cytokines in mice. BMC Complement Med Ther. 2020; 20(1):115. doi: 10.1186/s12906-020-02906-7
- Liu B, Fang Y, Yi R, Zhao X. Preventive Effect of Blueberry Extract on Liver Injury Induced by Carbon Tetrachloride in Mice. Foods. 2019 Feb 1;8(2):48. doi: 10.3390/foods8020048
- Lazic SE, Semenova E, Williams DP. Determining organ weight toxicity with Bayesian causal models: Improving on the analysis of relative organ weights. Sci Rep. 2020 Apr 20;10(1):6625. doi: 10.1038/s41598-020-63465-y
- Bencheikh N, Bouhrim M, Kharchoufa L, Choukri M, Bnouham M, Elachouri M. Protective Effect of Zizyphus lotus L. (Desf.) Fruit against CCl4-Induced Acute Liver Injury in Rat. Evid Based Complement Alternat Med. 2019 Dec 25;2019:6161593. doi: 10.1155/2019/6161593
- Shittu OK, Lawal B, Haruna GM, Berinyuy EB, Yusuf AA, Ibrahim AM. Hepato-curative effects of methanol extract from Nigerian Bee Propolis in carbon tetrachloride (CCl4) intoxicated rats. Eur. J. Biotechnol. Biosci. 2015; 3: 1-4.
- Gaim K, Gebru G, Abba S. The effect of arsenic on liver tissue of experimental animals (fishes and mice) – A review article. Int J Sci Res Publ. 2015; 5, 1-9.
- Kim WR, Flamm SL, Di Bisceglie AM, Bodenheimer HC. Public Policy Committee of the American Association for the Study of Liver Disease. Serum activity of alanine aminotransferase (ALT) as an indicator of health and disease. Hepatology. 2008; 47(4):1363-1370. doi: 10.1002/hep.22109
- Ebaid H, Bashandy SA, Alhazza IM, Rady A, El-Shehry S. Folic acid and melatonin ameliorate carbon tetrachloride-induced hepatic injury, oxidative stress and inflammation in rats. Nutr Metab (Lond). 2013; 10(1):20. doi: 10.1186/1743-7075-10-20
- Han CY, Sun TT, Xv GP, Wang SS, Gu JG, Liu CY. Berberine ameliorates CCl4 induced liver injury in rats through regulation of the Nrf2 Keap1 ARE and p53 signaling pathways. Mol Med Rep. 2019;20(4):3095-3102. doi: 10.3892/mmr.2019.10551
- Adewale OB, Adekomi DA, Muhameed OA. Neuronal alterations in the prefrontal cortex of rats with carbon tetrachloride (CCl4) induced hepatic damage. J. Clin. Pathol. Forensic Med. 2013; 4: 6-14. doi: 10.5897/JCPFM2013.0045
- Nguyen N, Le T, Do H, Ngo D, Le H, Truong N. Comparative treatment efficiency of adipose and bone marrow derived allogenic mesenchymal stem cell transplantation in mouse models of liver fibrosis. Biomed Res Ther. 2017; 4(6): 1374-1387.
doi: 10.15419/bmrat.v4i06.179 - Fernandez NJ, Kidney BA. Alkaline phosphatase: beyond the liver. Vet Clin Pathol. 2007; 36(3):223-233.
doi: 10.1111/j.1939-165x.2007.tb00216.x - Lazarov L. Markers for hepatocellular damage and affecting the biliary tract in the course of acute pancreatitis in dogs. Tradit. Mod. Vet. Med. 2021; 6: 3-10.
- Ibrahim EI, Enafie E, Farid AS. Star Anise (Illiciumverum) oil administration alleviates carbon tetrachloride-induced hepatotoxicity in rats. Benha Vet. Med. J. 2020; 39: 100-104. doi: 10.21608/bvmj.2020.51053.1303
- Lowe D, Sanvictores T, John S. Alkaline Phosphatase. In: StatPearls. Treasure Island (FL): StatPearls Publishing. 2022 Jan. Available at: https://www.ncbi.nlm.nih.gov/books/NBK459201/
- Amer MA, El-missiry MA, El-nabi AAR. The Role of Ficus carica leaf extract in modulation of the experimentally induced hepatotoxic damage in male rats. Int J Adv Res. 2015; 3: 572-585.
- Oratz M, Rothschild MA, Schreiber SS, Lane BP. Spermine stimulation of CCl4 depressed protein synthesis in rabbits. Gastroenterology. 1980 Dec;79(6):1165-1173. PMID: 7439626
- Yuchong Z, Xinyun Z, Yao W, Huijiao L, Chunyan Y, Shu J, Wenyue Z, Chunmei W, Jinghui S, He L, Jianguang C. Anwulignan alleviates carbon tetrachloride-induced acute liver injury in mice. Nat. Prod. Commun. 2020; 15: 1-8. doi: 10.1177/1934578X20962679
- Luedde T, Kaplowitz N, Schwabe RF. Cell death and cell death responses in liver disease: mechanisms and clinical relevance. Gastroenterology. 2014;147(4):765-783.e4. doi: 10.1053/j.gastro.2014.07.018
- Hassan SS, Elbakry MH, Mangoura SA, Omar ZM. Evaluation of the effect of Gallic acid against carbon tetrachloride- induced liver injury in albino rats: histological, immunohistochemical and biochemical study. J Med Histol. 2018; 1(2): 202-215.
doi: 10.21608/JMH.2017.7928 - Ayatollahi M, Hesami Z, Jamshidzadeh A, Gramizadeh B. Antioxidant effects of bone marrow mesenchymal stem cell against carbon tetrachloride-induced oxidative damage in rat livers. Int J Organ Transplant Med. 2014;5(4):166-173. PMID: 25426285
- Lai HY, Chou TY, Tzeng CH, Lee OK. Cytokine profiles in various graft-versus-host disease target organs following hematopoietic stem cell transplantation. Cell Transplant. 2012;21(9):2033-2045. doi: 10.3727/096368912X653110
- Ma T, Gong K, Ao Q, Yan Y, Song B, Huang H, Zhang X, Gong Y. Intracerebral transplantation of adipose-derived mesenchymal stem cells alternatively activates microglia and ameliorates neuropathological deficits in Alzheimer's disease mice. Cell Transplant. 2013;22 Suppl 1:S113-126. doi: 10.3727/096368913X672181
- Woodward EA, Prêle CM, Nicholson SE, Kolesnik TB, Hart PH. The anti-inflammatory effects of interleukin-4 are not mediated by suppressor of cytokine signalling-1 (SOCS1). Immunology. 2010; 131(1):118-127. doi: 10.1111/j.1365-2567.2010.03281.x
- Clarke RM, Lyons A, O'Connell F, Deighan BF, Barry CE, Anyakoha NG, Nicolaou A, Lynch MA. A pivotal role for interleukin-4 in atorvastatin-associated neuroprotection in rat brain. J Biol Chem. 2008;283(4):1808-1817. doi: 10.1074/jbc.M707442200
- Ponomarev ED, Maresz K, Tan Y, Dittel BN. CNS-derived interleukin-4 is essential for the regulation of autoimmune inflammation and induces a state of alternative activation in microglial cells. J Neurosci. 2007; 27(40):10714-10721.
doi: 10.1523/JNEUROSCI.1922-07.2007 - Volpin G, Cohen M, Assaf M, Meir T, Katz R, Pollack S. Cytokine levels (IL-4, IL-6, IL-8 and TGFβ) as potential biomarkers of systemic inflammatory response in trauma patients. Int Orthop. 2014; 38(6):1303-1309. doi: 10.1007/s00264-013-2261-2
- Li JF, Zhang DJ, Geng T, Chen L, Huang H, Yin HL, Zhang YZ, Lou JY, Cao B, Wang YL. The potential of human umbilical cord-derived mesenchymal stem cells as a novel cellular therapy for multiple sclerosis. Cell Transplant. 2014; 23 Suppl 1:S113-22.
doi: 10.3727/096368914X685005 - Chai NL, Zhang XB, Chen SW, Fan KX, Linghu EQ. Umbilical cord-derived mesenchymal stem cells alleviate liver fibrosis in rats. World J Gastroenterol. 2016; 22(26):6036-6048. doi: 10.3748/wjg.v22.i26.6036
- Jia Z, Li F, Zeng X, Lv Y, Zhao S. The effects of local administration of mesenchymal stem cells on rat corneal allograft rejection. BMC Ophthalmol. 2018;18(1):139. doi: 10.1186/s12886-018-0802-6
- Cantarelli E, Pellegrini S, Citro A, Sordi V, Piemonti L. Bone marrow- and cord blood-derived stem cell transplantation for diabetes therapy. CellR4. 2015. 3: 1-21. doi: 10.1.1.683.1503&rep=rep1&type=pdf
- Singh G, Korkaya H. Cytokine regulation of stem cells. Peer J Prepr. 2016. 4:e2347v1. doi: 10.7287/peerj.preprints.2347v1
- Nabekura T, Riggan L, Hildreth AD, O'Sullivan TE, Shibuya A. Type 1 Innate Lymphoid Cells Protect Mice from Acute Liver Injury via Interferon-γ Secretion for Upregulating Bcl-xL Expression in Hepatocytes. Immunity. 2020; 52(1):96-108.e9.
doi: 10.1016/j.immuni.2019.11.004 - Gala K, Burdzińska A, Idziak M, Wilczek E, Pączek L. Transplantation of mesenchymal stem cells into the skeletal muscle induces cytokine generation. Cytokine. 2013; 64(1):243-50. doi: 10.1016/j.cyto.2013.06.314
- Hoogduijn MJ, Roemeling-van Rhijn M, Engela AU, Korevaar SS, Mensah FK, Franquesa M, de Bruin RW, Betjes MG, Weimar W, Baan CC. Mesenchymal stem cells induce an inflammatory response after intravenous infusion. Stem Cells Dev. 2013; 22(21):2825-35.
doi: 10.1089/scd.2013.0193 - Lu X, Cui J, Cui L, Luo Q, Cao Q, Yuan W, Zhang H. The effects of human umbilical cord-derived mesenchymal stem cell transplantation on endometrial receptivity are associated with Th1/Th2 balance change and uNK cell expression of uterine in autoimmune premature ovarian failure mice. Stem Cell Res Ther. 2019; 10(1):214. doi: 10.1186/s13287-019-1313-y
- Resende RG, Correia-Silva JD, Silva TA, Xavier SG, Bittencourt H, Gomez RS, Abreu MH. Saliva and blood interferon gamma levels and IFNG genotypes in acute graft-versus-host disease. Oral Dis. 2012; 18(8):816-22. doi: 10.1111/j.1601-0825.2012.01955.x
- Nakamura H, Komatsu K, Ayaki M, Kawamoto S, Murakami M, Uoshima N, Yagi T, Hasegawa T, Yasumi M, Karasuno T, Teshima H, Hiraoka A, Masaoka T, Serum levels of soluble IL-2 receptor, IL-12, IL-18, and IFN-gamma in patients with acute graft-versus-host disease after allogeneic bone marrow transplantation. J Allergy Clin Immunol. 2000; 106:45-50. doi: 10.1067/MAI.2000.106774
- Xu J, Wei J, Zhu X, Zhang X, Guan J, Wang J, Yin J, Xiao Y, Zhang Y. Interferon- g Levels Correlate with the Severity of Acute Stem Cell Transplantation. Biol Blood Marrow Transplant. 2013; 19: 196-201.
- Larocca RA, Moraes-Vieira PM, Bassi EJ, Semedo P, de Almeida DC, da Silva MB, Thornley T, Pacheco-Silva A, Câmara NO. Adipose tissue-derived mesenchymal stem cells increase skin allograft survival and inhibit Th-17 immune response. PLoS One. 2013; 8(10):e76396. doi: 10.1371/journal.pone.0076396
- Wu J, Wang Q, Fu X, Wu X, Gu C, Bi J, Xie F, Kang N, Liu X, Yan L, Cao Y, Xiao R. Influence of Immunogenicity of Allogeneic Bone Marrow Mesenchymal Stem Cells on Bone Tissue Engineering. Cell Transplant. 2016;25(2):229-42. doi: 10.3727/096368915X687967
- Piryaei A, Valojerdi M, Shahsavani M, Baharvand H. differentiation of bone marrow-derived mesenchymal stem cells into hepatocyte-like cells on nanofibers and their transplantation into a carbon tetrachloride-induced liver fibrosis. Stem Cell Rev Rep. 7, 103-118 (2011). doi: 10.1007/s12015-010-9126-5
- Spees JL, Lee RH, Gregory CA, Mechanisms of mesenchymal stem / stromal cell function. Stem Cell Res. Ther. 7, 1=13 (2016).
doi: 10.1186/s13287-016-0363-7
Accepted 28 January 2022


