Platelet lysate for rapid expansion of human mesenchymal stromal cells
Claudia Lange, Figen Cakiroglu, Andrej Spiess, Heike Cappallo-Obermann, Axel R. Zander
Clinic for Stem Cell Transplantation, University Hospital Hamburg-Eppendorf, Martinistr. 52, 20246 Hamburg, Germany
Correspondence:
Claudia Lange, Clinic for Stem Cell Transplantation, University Hospital Hamburg-Eppendorf, Martinistr. 52, 20246 Hamburg, Germany,
E-mail: cllange@uke.uni-hamburg.de
Accepted 07 November 2008
Published 01 December 2008
Summary
Human bone marrow mesenchymal stromal cells (hMSC) are promising candidates for new treatment options in transplant and regenerative medicine. However, most expansion protocols still use fetal calf serum (FCS) as growth factor supplement, which is a potential source of undesirable xenogeneic pathogens. We established an easy and reproducible expansion protocol for hMSC based on the addition of platelet lysate (PL) obtained from human thrombocyte concentrates. Both CFU-F and cumulative cell numbers were significantly increased compared to the conventional FCS-based medium. The generated cells meet all criteria for MSCs, e.g. plastic adherence, spindle-shaped morphology, surface marker expression, lack of hematopoietic markers, and differentiation capability into 3 mesenchymal lineages. Human MSC expanded with PL revealed favorable immunological properties in vitro. Gene expression profiles showed upregulation of cell cycle and DNA replication genes and downregulation of developmental, differentiation, adipogenic and MHC II genes. Thus, PL provides a safe component for accelerated and safe hMSC expansion.
Keywords
Mesenchymal stromal cells, platelet lysate, growth factor, gene expression
Introduction
Multipotent mesenchymal stromal cells (MSC), also named mesenchymal stem cells, are characterized by adherence to plastic when maintained in standard cultures in vitro, by expression of surface antigens CD105 and CD90 but lack of hematopoietic markers CD34 and CD45, and by differentiation into osteoblasts, adipocytes and chondroblasts in vitro [1]. Since their first description [2], a multitude of work has been carried out to show their properties and functionality in vitro and in vivo [3, 4, 5]. MSC have been shown to display a considerable therapeutic potential in pre-clinical [6-11] and clinical [12-16] studies for the treatment/regeneration of neuronal degeneration, osteogenesis imperfecta, graft-versus-host disease, support of hematopoietic engraftment, metabolic diseases, and bone and cartilage tissues, as well as renal and myocardial infarction. To date, all reported clinical trials are employing hMSC generated in medium supplemented with fetal calf serum (FCS). FCS, however, is a source of undesirable xenogeneic antigens, and carries the risk of transmitting animal viral, prion and zoonose contaminations. Additionally, FCS has been implicated with anaphylactic or arthus-like immune reactions in patients who received cells generated in FCS-supplemented medium [17], even leading to arrhythmias after cellular cardioplasty [18]. Uptake of FCS components is an active process [19]. Although up to 99.99% of FCS can be removed by sequential cultivation of MSC first in FCS, followed by autologous or heterologous serum [20], a residual risk still remains.
Very recently, human platelet lysates (PL) have been shown to serve as a safe substitute for animal serum for hMSC expansion [21-23], but the resulting hMSC are still not fully characterized. We have extensively analyzed animal-serum free culture conditions for hMSC expansion using platelet lysate as a substitute for FCS. Compared to FCS-supplemented culture conditions, we found a significant increase of both CFU-F as well as cumulative cell numbers after expansion. Our optimized protocol uses 5% of PL as growth supplement. Cells obtained by this protocol meet all criteria for MSCs, e.g. plastic adherence, spindle-shaped morphology, surface marker expression, lack of hematopoietic markers, and differentiation capability into 3 mesenchymal lineages. MSC retained their immune-privileged potential by suppressing the allogeneic reaction of T-cells. Additionally, gene expression profiles showed decreased mRNA levels of MHC II components. Taken together, our GMP-compatible protocol allows for safe and accelerated expansion of hMSC, which could be of interest for cell and tissue therapies.
Results and discussion
In comparing the additives FCS and PL, the media used consisted of α-MEM containing glutamax, the stable form of glutamine, supplemented either with + 10% preselected fetal calf serum (FCS; BioWhittaker, Apen, Germany) + 1% glutamine or 5% freshly thawed platelet lysate (PL) + 10 IU Heparin (Roche, Grenzach-Wylen, Germany; 5000 IU/ml) per 5 ml medium. The isolation of hMSC already revealed a higher number of CFU-F in PL-containing medium (Table 1) as well as larger colonies (Figure 1). In line with the CFU-F numbers, the expansion capabilities of hMSC grown in PL were considerably higher (Figure 2), reaching twice as many cells after only 40 days. With regard to morphology, a more elongated cell appearance has been observed in PL-cultures, resulting in significantly higher cell numbers per growth area.
Table 1. Isolation of hMSC with FCS- or PL-supplemented media.
Values are shown for 107 plated cells.

Figure 1. Isolation of hMSC by plating 5 x 105 mononuclear cells/well in 3 ml.
Shown are crystal violet-stained CFU-F in FCS- or PL-supplemented media 14 days after seeding.

Figure 2. Accelerated expansion of MSC in PL- compared to FCS-containing medium αMEM.
Shown are cumulative cell numbers of one example out of 11 experiments. Each symbol respresents a single time point of trypsinization.

PL contains 7 fundamental growth factors actively secreted by platelets: PDGF-αα (platelet derived growth factor), -ββ, -αβ, TGF-β1 (transforming growth factor) and -β2, VEGF (vascular endothelial growth factor) and EGF (epidermal growth factor) [24, 25]. The growth factors PDGF, TGF, EGF and FGF (fibroblast growth factor) have been described as mitogens for MSC [4]. Thrombocyte concentrates are regularly produced and applied in everyday clinical life, and meet all criteria for a safe and well-controlled growth factor source. The main reason for the superiority of PL therefore may originate in the release of these factors. We thoroughly analyzed PL with either Human 27-plex (BIO-RAD) or ELISA and showed that inflammatory and anti-inflammatory cytokines as well as a variety of mitogenic factors are contained in PL (Table 2). Previously, it has been shown that thrombocytes release certain amounts of mitogenic cytokines, varying for PDGF-αβ for example, between 35-133 ng/ml [25]. For effective expansion of MSC, an optimized preparation of PL is needed. It consists of pooled PL from at least 10 donors (to equalize for differences in cytokine concentrations) with a minimum concentration of 3 x 109 thrombocytes/ml. Beside this, the accelerated growth under the influence of PL is supported by differential gene expression profile showing an upregulation of cycle-promoting proteins and downregulation of genes for differentiation, attachment, and apoptosis [26].
Table 2. Determination of factor-concentrations in PL. Anti-inflammatory cytokines are shown in bold, inflammatory in italic.
The human-plex method presents the concentration in [pg/ml] from undiluted PL, while in the ELISA PL was diluted to a thrombocyte concentration of 1 x 109/ml and used as 5% in medium (the values therefore have to be multiplied by at least 20). < : below the detection limit.

Evaluation of the surface antigens CD34, CD45, CD59, CD90 and CD105 by flow cytometry revealed a similar phenotype as with FCS-medium, i.e. a lack of the hematopoietic markers CD34 and CD45 and expression of CD59, CD90 and CD105 (not shown). Additionally, both expansion media enabled a subsequent differentiation of hMSC into osteo-, adipo- and chondrogenic lineages. An exception in the quantity of differentiating cells was found for adipogenic differentiation. The formation of adipocytes was delayed and required longer induction times. This result is supported by the downregulation of genes involved in fatty acid metabolism [26]. We assess this decreased adipogenic/lipogenic ability as a favorable property, because in mice the intra-arterial injection of MSC for treatment of chronic kidney injury has revealed formation of adipocytes [27].
MSC have been described as immunomodulatory by impairing T-cell activation without inducing anergy. We tested the immunomodulatory properties of PL-expanded hMSC in vitro in the mixed lymphocyte reaction (MLR). MLRs were carried out with different combinations of allogeneic human peripheral blood mononuclear cells (hPBMC) used as effectors (E) and irradiated stimulators/activators (A) at ratios of 1:1. Human MSC (M) added to the MLR were from unrelated healthy donors. In all 6 experiments, hMSC added at effector/stimulator/MSC ratio of 1:1:1 suppressed T cell proliferation efficiently (p=0.000004). The average inhibition at this ratio was 84.8 ± 9.7% (Figure 3). In contrast to FCS-generated hMSC, no dilution effect of the MSC-effect with decreasing numbers [28] was observed. This result is supported by differential gene expression showing a downregulation of MHC II compounds in hMSC (Figure 4). Addition of PL-generated hMSC leads to significantly decreased immunostimulation of allogeneic T cells caused by MSC. Expanded hMSC express MHC I but not II complexes although MHC II is present intracellularly, and can be induced by addition of interferon gamma (IFN-γ) [29]. The lack of MHC II on hMSC has been interpreted so far as evidence for their non-stimulating properties, so that MSC are transplantable between MHC-incompatible individuals. The downregulation of MHC II in hMSC expanded in PL-supplemented medium makes the cell preparations even more safe and useful for application in cell-replacement therapies. It has been shown that both autologous and allogeneic MSC can be used without significant immune reactions [30, 31, 32] and PL-MSC could make the allogeneic use even safer. We expect, according to the results of decreased allo-stimulation under the influence of PL-MSC, a broader applicability of these MSC.

Figure 3. Immunomodulatory properties of hMSC are preserved after cultivation in PL-supplemented medium. Bar graph shows the relative percentage of Ki-67+ CD3+ cells in the presence of effector (E), irradiated activator (A), and PL-generated MSCs (M) in various ratios. Data represent relative mean values ± SD of proliferating Ki-67 positive T-cells from 6 experiments.
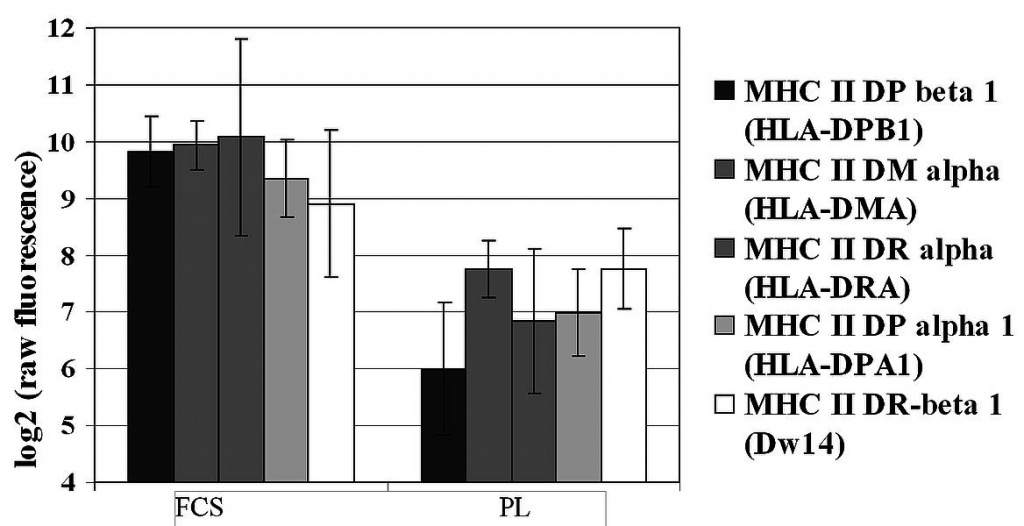
Figure 4. Differential gene expression profile reveals the downregulation of MHC II compounds in MSCs cultured in PL- compared to FCS-supplemented media.
Gene expression values are shown as log2 of raw fluorescence for MHC II genes involved in antigen presentation.
Additional gene expression data shows that PL-generated MSCs might be particularly good candidates for regenerative therapy in CNS damage. They express the gene Prickle1, which is involved in neuro-regeneration, to an eight-fold higher degree when compared to MSCs cultured in FCS-supplemented media. Mouse Prickle1 and Prickle2 are expressed in postmitotic neurons and promote neurite outgrowth [33]. Furthermore, MAG (Myelin-associated glycoprotein) is expressed at 13-fold lower amount. MAG is a cell membrane glycoprotein, and may be involved in myelination during nerve regereneration. The lack of recovery after central nervous system injury is caused, in part, by myelin inhibitors including MAG. MAG acts as a neurite outgrowth inhibitor for most neurons tested, but stimulates neurite outgrowth in immature dorsal root ganglion neurons [34]. These differentially regulated genes would favor the use of PL-cultured hMSC for regeneration of neuronal injury. Additionally, the 12-fold higher expression of RAR (retinoid acid receptor) -responsive 1 gene (TIG1) [35], 9-fold higher expression of Keratin 18 [36], 5.7-fold higher expression of the cellular retinol binding protein 1 CRBP1 [37], and Prickle 1 suggest a less tumorigenic phenotype of the MSCs after cultivation in PL-supplemented media.
Conclusions
Isolation and expansion of hMSC using PL as medium supplement allows for rapid generation of high cell amounts within short time. MSC expanded under these conditions fulfill all criteria stated for hMSC. Differential gene expressions support the findings of delayed adipogenesis and favorable immunological properties. Thus, PL-generated hMSC are prime candidates for transplantation as well as regenerative approaches.
Acknowledgement
The work was supported by the Federal Ministry of Education and Research, Contract grant number 13N8904 (HyCelex).
References
1. Dominici M, Le Blanc K, Mueller I, Slaper-Cortenbach I, Marini F, Krause D, Deans R, Keating A, Prockop DJ, Horwitz E. Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy. 2006;8:315-317.
2. Friedenstein AJ, Deriglasova UF, Kulagina NN, Panasuk AF, Rudakowa SF, Luria EA, Ruadkow IA. Precursors for fibroblasts in different populations of hematopoietic cells as detected by the in vitro colony assay method. Exp Hematol. 1974;2:83-92.
3. Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, Mosca JD, Moorman MA, Simonetti DW, Craig S, Marshak DR. Multilineage potential of adult human mesenchymal stem cells. Science. 1999;284:143-147.
4. Deans RJ, Moseley AB. Mesenchymal stem cells: biology and potential clinical uses. Exp Hematol. 2000;28:875-884.
5. Fibbe WE, Noort WA. Mesenchymal stem cells and hematopoietic stem cell transplantation. Ann N Y Acad Sci. 2003;996:235-244.
6. Kopen GC, Prockop DJ, Phinney DG. Marrow stromal cells migrate throughout forebrain and cerebellum, and they differentiate into astrocytes after injection into neonatal mouse brains. Proc Natl Acad Sci U S A. 1999;96:10711-10716.
7. Mahmood A, Lu D, Chopp M. Marrow stromal cell transplantation after traumatic brain injury promotes cellular proliferation within the brain. Neurosurgery. 2004;55:1185-1193.
8. Petite H, Viateau V, Bensaid W, Meunier A, de Pollak C, Bourguignon M, Oudina K, Sedel L, Guillemin G. Tissue-engineered bone regeneration. Nat Biotechnol. 2000;18:959-963.
9. Lange C, Togel F, Ittrich H, Clayton F, Nolte-Ernsting C, Zander AR, Westenfelder C. Administered mesenchymal stem cells enhance recovery from ischemia/reperfusion-induced acute renal failure in rats. Kidney Int. 2005;68:1613-7.
10. Togel F, Hu Z, Weiss K, Isaac J, Lange C, Westenfelder C. Administered mesenchymal stem cells protect against ischemic acute renal failure through differentiation-independent mechanisms. Am J Physiol Renal Physiol. 2005;289:F31-42.
11. Jaquet K, Krause KT, Denschel J, Faessler P, Nauerz M, Geidel S, Boczor S, Lange C, Stute N, Zander A, Kuck KH. Reduction of myocardial scar size after implantation of mesenchymal stem cells in rats: what is the mechanism? Stem Cells Dev. 2005;14:299-309.
12. Horwitz EM, Prockop DJ, Fitzpatrick LA, Koo WW, Gordon PL, Neel M, Sussman M, Orchard P, Marx JC, Pyeritz RE, Brenner MK. Transplantability and therapeutic effects of bone marrow-derived mesenchymal cells in children with osteogenesis imperfecta. Nat Med. 1999;5: 309-313.
13. Le Blanc K, Rasmusson I, Sundberg B, Gotherstrom C, Hassan M, Uzunel M, Ringden O. Treatment of severe acute graft-versus-host disease with third party haploidentical mesenchymal stem cells. Lancet. 2004;363:1439-1441.
14. Koc ON, Gerson SL, Cooper BW, Dyhouse SM, Haynesworth SE, Caplan AI, Lazarus HM. Rapid hematopoietic recovery after coinfusion of autologous-blood stem cells and culture-expanded marrow mesenchymal stem cells in advanced breast cancer patients receiving high-dose chemotherapy. J Clin Oncol. 2000;18:307-316.
15. Koc ON, Day J, Nieder M, Gerson SL, Lazarus HM, Krivit W. Allogeneic mesenchymal stem cell infusion for treatment of metachromatic leukodystrophy (MLD) and Hurler syndrome (MPS-IH). Bone Marrow Transplant. 2002;30:215-222.
16. Chen SL, Fang WW, Ye F, Liu YH, Qian J, Shan SJ, Zhang JJ, Chunhua RZ, Liao LM, Lin S, Sun JP. Effect on left ventricular function of intracoronary transplantation of autologous bone marrow mesenchymal stem cell in patients with acute myocardial infarction. Am J Cardiol. 2004;94:92-95.
17. Selvaggi TA, Walker RE, Fleisher TA. Development of antibodies to fetal calf serum with arthus-like reactions in human immunodeficiency virus-infected patients given syngeneic lymphocyte infusions. Blood. 1997;89:776-779.
18. Chachques JC, Herreros J, Trainini J, Juffe A, Rendal E, Prosper F, Genovese J. Life-threatening arrhythmias after cellular cardioplasty. Autologous human serum for cell culture avoids the implantation of cardioverter-defibrillators in cellular cardiomyoplasty. Int J Cardiol. 2004;95, Suppl 1:S29-33.
19. Gregory CA, Reyes E, Whitney MJ, Spees JL. Enhanced engraftment of mesenchymal stem cells in a cutaneous wound model by culture in allogenic species-specific serum and administration in fibrin constructs. Stem Cells. 2006;24:2232-2243.
20. Spees JL, Gregory CA, Singh H, Tucker HA, Peister A, Lynch PJ, Hsu SC, Smith J, Prockop DJ. Internalized antigens must be removed to prepare hypoimmunogenic mesenchymal stem cells for cell and gene therapy. Mol Ther. 2004;9:747-756.
21. Yamada Y, Ueda M, Hibi H, Nagasaka T. Translational Research for Injectable Tissue-Engineered Bone Regeneration Using Mesenchymal Stem Cells and Platelet-Rich Plasma: From Basic Research to Clinical Case Study. Cell Transplantation. 2004;13:343-355.
22. Doucet C, Ernou I, Zhang Y, Llense JR, Begot L, Holy X, Lataillade JJ. Platelet lysates promote mesenchymal stem cell expansion: a safety substitute for animal serum in cell-based therapy applications. J Cell Physiol. 2005;205:228-236.
23. Muller I, Kordowich S, Holzwarth C, Spano C, Isensee G, Staiber A, Viebahn S, Gieseke F, Langer H, Gawaz MP, Horwitz EM, Conte P, Handgretinger R, Dominici M. Animal serum-free culture conditions for isolation and expansion of multipotent mesenchymal stromal cells from human BM. Cytotherapy. 2006;8:437-444.
24. Marx RE, Carlson ER, Eichstaedt RM, Schimmele SR, Strauss JE, Georgeff KR. Platelet-rich plasma: Growth factor enhancement for bone grafts. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 1998;85:638-646.
25. Marx RE. Platelet-rich plasma: evidence to support its use. J Oral Maxillofac Surg. 2004;62:489-496.
26. Lange C, Cakiroglu F, Spiess AN, Cappallo-Obermann H, Dierlamm J, Zander AR. Accelerated and safe expansion of human mesenchymal stromal cells in animal serum-free medium for transplantation and regenerative medicine. J Cell Physiol. 2007;25:18-26.
27. Kunter U, Rong S, Boor P, et al. Mesenchymal stem cells prevent progressive experimental renal failure but maldifferentiate into glomerular adipocytes. J Am Soc Nephrol. 2007 Jun;18(6):1754-64).
28. Fang L, Lange C, Engel M, Zander AR, Fehse B. Sensitive Balance of Suppressing and Activating Effects of MSC on T Cell Proliferation. Transplantation. 2006;82:1370-1373.
29. Le Blanc K, Tammik C, Rosendahl K, Zetterberg E, Ringden O. HLA expression and immunologic properties of differentiated and undifferentiated mesenchymal stem cells. Exp Hematol. 2003;31:890-896.
30. Poh KK, Sperry E, Young RG, Freyman T, Barringhaus KG, Thompson CA. Repeated direct endomyocardial transplantation of allogeneic mesenchymal stem cells: Safety of a high dose, "off-the-shelf", cellular cardiomyoplasty strategy. Int J Cardiol Aug. 2006;2; [Epub ahead of print]
31. Ringden O, Uzunel M, Rasmusson I, Remberger M, Sundberg B, Lonnies H, Marschall HU, Dlugosz A, Szakos A, Hassan Z, Omazic B, Aschan J, Barkholt L, Le Blanc K. Mesenchymal stem cells for treatment of therapy-resistant graft-versus-host disease. Transplantation. 2006;81:1390-1397.
32. Dai W, Hale SL, Martin BJ, Kuang JQ, Dow JS, Wold LE, Kloner RA. Allogeneic mesenchymal stem cell transplantation in postinfarcted rat myocardium: short- and long-term effects. Circulation. 2005;112:214-223.
33. Okuda H, Miyata S, Mori Y, Tohyama M. FEBS Lett. 2007;581:4754-60.
34. Vyas AA, Patel HV, Fromholt SE, Heffer-Lauc M, Vyas KA, Dang J, Schachner M, Schnaar RL. Gangliosides are functional nerve cell ligands for myelin-associated glycoprotein (MAG), an inhibitor of nerve regeneration. Proc Natl Acad Sci U S A. 2002;99:8412-7.
35. Liang Y, Jansen Mi, Aronow B, Geiger H, Van Zant G. The quantitative trait gene latexin influences the size of the hematopoietic stromal cell population in mice. Nature Genetics. 2007;39:178-188.
36. Bühler H, Schaller G. Transfection of keratin 18 gene in human breast cancer cells causes induction of adhesion proteins and dramatic regression of malignancy in vitro and in vivo. Mol Cancer Res. 2005;3:365-71.
37. Roberts D, Williams SJ, Cvetkovic D, Weinstein JK, Godwin AK, Johnson SW, Hamilton TC. Decreased expression of retinol-binding proteins is associated with malignant transformation of the ovarian surface epithelium. DNA Cell Biol. 2002;21:11-9.
Accepted 07 November 2008
Published 01 December 2008


